The past few blog posts have been about manual lymph drainage (MLD) and contraindications. When appropriately used, MLD is a modality that has several health benefits. But that’s only when the technique is properly applied.
MLD is a specialized massage designed to stimulate the lymphatic system and promote the movement of lymph fluid. Effective MLD requires an understanding of lymphatic anatomy and biomechanics. Proper technique is critical, as excessive pressure can compromise the delicate structure of initial lymph capillaries, leading to ineffective drainage or structure damage. These capillaries rest beneath the skin’s surface in the dermis layer where there are blood vessels and nerves.
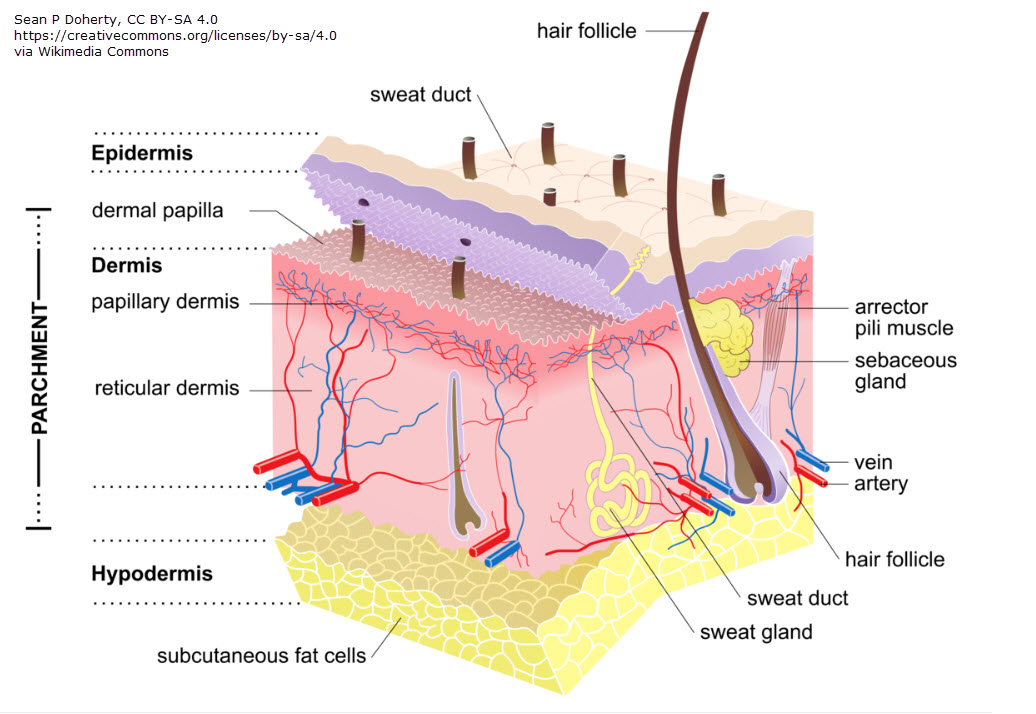
Lymph Capillary Anatomy
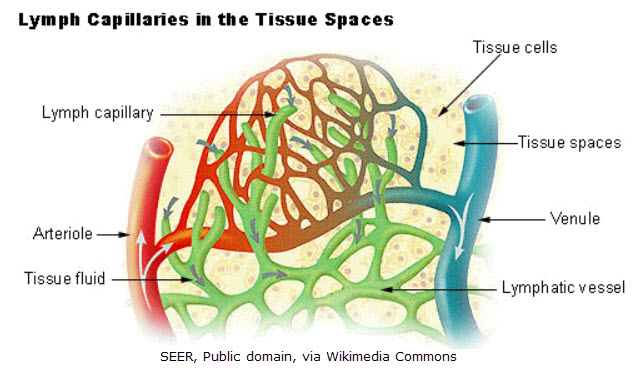
The initial lymph capillaries form the entry point for interstitial fluid (fluid in the tissue space) to enter into the lymphatic system. Unlike blood capillaries, they possess unique structural characteristics that make them highly specialized for fluid uptake:
- Endothelial Structure: The walls of initial lymph capillaries consist of a single layer of overlapping endothelial cells, creating valve-like openings that allow fluid entry. (Deeper lymphatic structures contain smooth muscle, but these superficial structures do not.)
- Anchoring Filaments: These fine thread-like initial lymph capillaries attach lymphatic endothelial cells to surrounding connective tissue. They play a crucial role in preventing capillary collapse and facilitating fluid movement in response to interstitial pressure changes. Anchoring filament diameter is around 20 to 30 nanometers.3
- Diameter and Fragility: Initial lymph capillaries are extremely delicate, with diameters ranging from 10 to 60 microns.5 Their thin walls and flexible structure make them highly responsive but also vulnerable to mechanical stress. (According to Foldi, “A gentle and careful touch is indicated, since the lymph vessels affected by MLD are less than one millimeter in diameter on average. The more superficial, valveless lymph capillaries as well as the precapillary channels are even smaller in diameter.”)4
Why Excessive Pressure in MLD Can Be Harmful
MLD should be performed with light, rhythmic movements to optimize fluid mobilization without causing harm. It’s just enough pressure to stretch the skin and not slide, typically around 20-30 mmHg or less.1 This pressure is significantly lower than typical massage techniques, as the goal is not to manipulate the muscles but to gently stimulate the lymphatic vessels. Applying too much pressure can result in the following complications:
- Capillary Compression and Closure: Due to their fragile nature, lymph capillaries can collapse under excessive pressure, preventing fluid entry and impeding drainage.
- Damage to Anchoring Filaments: These filaments are highly sensitive to mechanical force. Excessive pressure can rupture them, reducing the efficiency of fluid uptake and leading to localized edema.
- Increased Interstitial Pressure: Heavy-handed techniques may inadvertently increase interstitial pressure, pushing fluid back into tissues rather than facilitating its movement into lymphatic capillaries.
(It’s important to note, there are times such as when dealing with fibrosis that this light pressure may need to be firmer.)
Principles of Effective MLD1
To maximize the effectiveness of MLD and protect the integrity of lymphatic structures, practitioners should adhere to the following principles:
- Gentle, rhythmic movements applied at a rate of about 1/sec, with 5–7 repetitions per area. The pressure is gentle and light (typically 20-30 mmHg or less)2 to ensure the capillaries remain open and receptive to fluid intake. The motions are predominately circular and done to stretch the skin which, in turn, stretches the lymphangion wall and increases lymphangiomotion (the contractions of lymphangions, the deeper lymph vessels which contain smooth muscle).
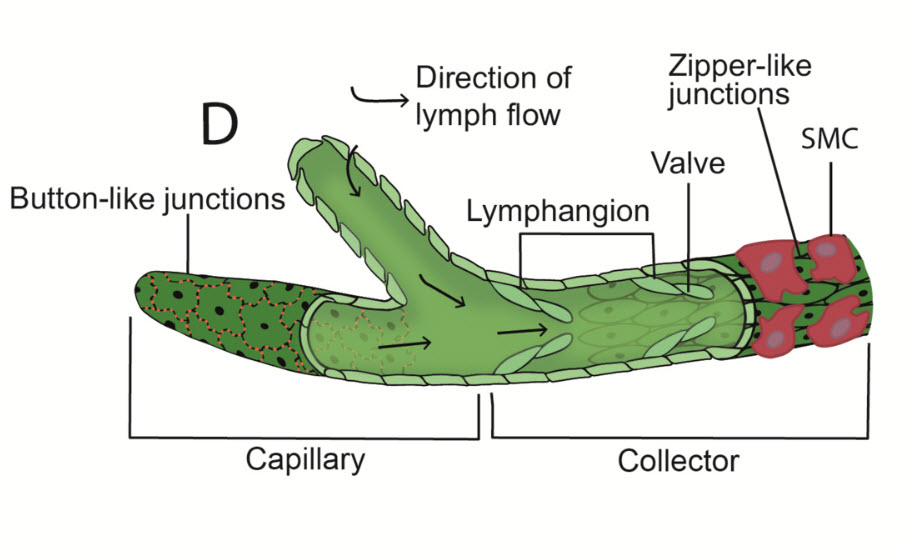
- Use of a pressure phase, which promotes movement of fluid in the desired drainage direction, and a pressure-free or relaxation phase, in which a vacuum caused by passive distention of the tissue leads to refilling of the lymph vessels from the periphery (Vodder’s “suction effect”).
- Directing lymph flow by starting proximally and moving distally. MLD follows a specific sequence, starting with the clearing of proximal areas (nearer to the trunk) to ensure that distal areas (farther from the trunk) can effectively drain. The sequence also follows the anatomical pathways of lymphatic drainage, guiding fluid toward functioning lymph nodes (via normal pathways – or rerouting fluid to healthy pathways when there is damage).
- Use of slow, repetitive strokes. MLD is most effective when performed with consistent, repetitive motions that mimic the natural pumping action of the lymphatic system. This also creates a relaxation effect.
By understanding the delicate nature of initial lymph capillaries and applying appropriate MLD techniques, therapists can optimize lymphatic function while avoiding potential harm. Proper execution, as described in Dr. Földi and Dr. Vodder’s text, ensures that MLD remains a safe and effective therapy for individuals managing lymphedema and other lymphatic disorders.
References
1 Földi, Michael; Földi, Ethel; Strößenreuther, Cornelia; Kubik, Stefan. Földi’s Textbook of Lymphology: for Physicians and Lymphedema Therapists (German Edition) (pp. 1360-1361). Elsevier Health Sciences. Kindle Edition.
2 Near-infrared fluorescence lymphatic imaging to reconsider occlusion pressure of superficial lymphatic collectors in upper extremities of healthy volunteers. J Lymphology. 2024; 39(4):234-245. doi:10.xxxx/j.lymph.2024.234
3 Schmid-Schönbein GW, Pusateri AE, Yao L. Structural characteristics and functions of lymphatic capillaries. Microcirculation. 2003;10(4):315-328. doi:10.1080/10739680390179253.
4 Földi, Michael; Földi, Ethel; Strößenreuther, Cornelia; Kubik, Stefan. Földi’s Textbook of Lymphology: for Physicians and Lymphedema Therapists (German Edition) (p. 1430). Elsevier Health Sciences. Kindle Edition.
5 Schmid-Schönbein GW. Microlymphatics and lymph flow. Physiol Rev. 1990;70(4):987-1028. doi:10.1152/physrev.1990.70.4.987
