If you or your doctor decide you need to see a therapist for lymphedema, what should you expect? And if you do get treatment, will it work?
In the Beginning
The first session will be an evaluation to assess the status of your lymphedema. A therapist will gather background information such as your past medical history and take baseline measurements. They may also take photos (particularly if you have wounds). This session will enable the therapist to establish a plan of care outlining what they plan to do to in treatment and collaborate with you on goals.
Phase I – Complete Decongestive Therapy

Subsequent sessions will involve treatment and education. This is Phase 1. Treatment for lymphedema is complete decongestive therapy (CDT) which includes manual lymph drainage, bandaging, skin care and exercise. Let’s look at each one of these components.
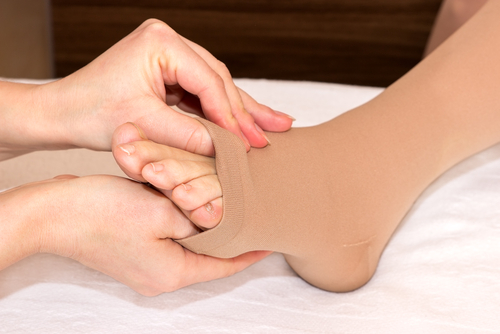
(Hands Massage photo by Andreas 160578-Pixabay)
- Manual lymph drainage is a medical massage used to stimulate lymphatic fluid movement. It is used to decongest the swollen area and re-route fluid to healthy lymph nodes when appropriate. It’s a slow, rhythmic manual technique that has numerous benefits outside of lymphedema for general health and wellness. But in this case, it is specifically used to remove stagnant lymph fluid causing swelling in an extremity. The massage is also very gentle and light so as to avoid damaging the fragile lymphatic vessels that sit near the skin’s surface. The exception is when there is fibrotic tissue (tissue that has become firm due to congestion and inflammation caused by a damaged or impaired lymphatic system.
- Bandaging is an essential part of treatment. It is done with several layers of special bandages called short-stretch bandages (this type of compression bandage stretches a short distance when pulled). These are applied over a padding layer and provide resistance during movement or exercise. The bandages help break down fibrotic tissue and stimulate lymph movement. But they also prevent fluid that has been removed from refilling an area that is being decongested.
- Skin care is important because your skin is a barrier to bacteria. And skin changes are seen in lymphedema as the condition progresses. Initially, skin becomes thicker. Later papules (bumps), hyperkeratosis (excess skin growth), discoloration and other skin changes can occur. As this continues, your risk of a cellulitis infection goes up. Education about appropriate skin products and skin protection should be a component of skin care.
- Exercise promotes lymph movement through muscle pumping action. While most any movement is beneficial, deep breathing and use of the involved extremity will likely be part of your exercise program.
Phase 2 – Maintenance
At the end of treatment, you will need a compression garment for maintenance (most likely one for daytime and another for night use). This is Phase 2. Some therapists will fit you for these, but many therapists will refer you to someone else who specializes in fitting garments.
The above is the gold standard and conservative treatment for lymphedema. The next question is: Does treatment work? While there is anecdotal evidence, fortunately, there is scientific research backing the claims of CDT and the individual components of this treatment (and has been for many years).1-3
Once in a while, treatment may not be effective. Why would this be? We’ll look at that next time.
References
1 Michopoulos E, Papathanasiou G, Vasilopoulos G, Polikandrioti M, Dimakakos E. Effectiveness and Safety of Complete Decongestive Therapy of Phase I: A Lymphedema Treatment Study in the Greek Population. Cureus. 2020;12(7):e9264. Published 2020 Jul 19. doi:10.7759/cureus.9264
2 Foldi Textbook of Lymphology
3 Lymphedema A Concise Compendium of Theory and Practice